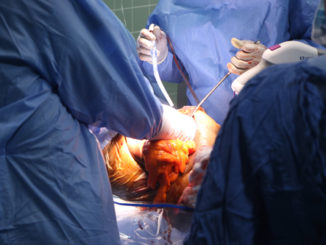
Liver cancer patients in the country can now get respite as the Korle Bu Teaching Hospital (KBTH) is now in a position to conduct successful surgeries to remove the cancerous parts of the liver, pancreas and bile duct.
Led by Dr Asare K. Offei, one of the two Ghanaian hepatobiliary (liver) surgeons, the KBTH has over the past one-and-half years successfully performed 120 surgeries and is now poised to conduct further surgeries at relatively lower cost.
Last Friday, this reporter was privileged to witness the latest of such surgeries performed on a 67-year-old woman at the hospital.
That Friday surgery marked another major breakthrough at the KBTH, offering hope to many patients who would otherwise have had to seek medical treatment abroad, if financially capable, or die within a short time from the illness.
After leading his team to perform the five-hour surgery, Dr Offei told the Daily Graphic that the hospital was capable of treating patients with liver, pancreas and bile duct cancer diseases.
The hospital had, in the past, successfully undertaken bladder reconstruction, key-hole surgery, re-attachment of a severed hand and a kidney transplant.
Cases
For almost one-and-a-half years Dr Offei and his team have seen more than 400 cases of liver, bile duct and pancreas conditions.
Dr Offei explained that in most cases the patients reported late, for which reason surgery could not be performed because the patients were in their terminal stages.
From the initial one case a month, he said, the team now performed two to four surgeries a week.
According to him, until the introduction of the whipples procedure in Ghana, which provides long-term survival for patients with pancreatic head cancer, such patients had limited survival within three months.
Challenges
Dr Offei said with the surgical capability currently available, coupled with technology, patients would have better chances of survival if they reported early for surgical intervention in hospital.
He explained that currently there was no specialist surgical clinic attending to patients with liver, bile duct and pancreatic problems, saying those patients were being handled at the general surgical clinic.
Dr Offei said some of the cases were often referred late but was hopeful that when a specialist clinic was set up, it would offer those patients shorter appointment times and prompt management.
He said he had put together a dedicated team of nurses, surgeons, anaesthetists, radiologists and gastroenterologist for the care of those patients.
He explained that a dedicated team was required because it was a specialised area of medicine that required a team to handle patients, equipment and consumables to ensure quality and safety of care for patients.
Cost
Dr Offei said it cost between GH¢10,000 and GH¢15,000 to perform one of such surgeries in Ghana, as against between $10,000 and $20,000 in some of the cheapest centres around the world.
The cost outside does not include flight and accommodation expenses for patients and accompanying relations.
He explained that because the unit had not been appropriately set up, patients had to purchase most of the items needed for their treatment outside the hospital.
But Dr Offei said if the hospital decided to set up the specialised unit and provide all needed inputs, the cost of the surgery would be cheaper for patients.
Team members
Currently, the team comprises Dr Asare K. Offei – hepatobiliary surgeon; Dr Fred Osei – consultant anaesthetist; Dr Samuel Essoun – consultant surgeon; Mr Prince Kwame Amponsah, Ms Regina Hayford, Ms Jemima Akwetey and Mr Kwaku Frimpong – peri-operative nurses.
Others are Mr Emmanuel Kumi Nyarko and Mr Stephen Narkotey – critical care nurses; Dr Andrea Appau – radiologist; Dr Benjamin Dabo Sarkodie – interventional radiologist; Dr Adwoa Agyei, Dr Kenneth Tachi and Dr Timothy Archeampong – gastroenterologists, and Mr Edward Tamekloe – administrative assistant.
The team is supported by dedicated residents and surgeons from the Department of Surgery.
Procedure
Dr Offei explained that there were eight regions of the liver, each with a dedicated source of blood supply.
He said with a CT scan, the team was able to identify the exact location of the cancer in the liver.
Dr Offei said one needed 30 per cent of the liver volume to survive (at least two or more of the eight regions), hence an assessment was made to determine if the patient would have enough remnant liver to survive before going ahead with the surgery.
He said with the advent of technology, his team did most of the surgeries without blood transfusion.
Cause
He said with the high prevalence rate of the Hepatitis B virus in Ghana (13 per cent), it was important that a campaign was launched to educate the population on the risk factors and for them to seek early treatment, especially if one tested positive.
He said when people were diagnosed of jaundice, it was important that they seek specialist attention to avoid further deterioration and liver failure.
Dr Offei said a non-governmental organisation, the Liver Cancer Foundation (www.livercancerfoundation.org), had been undertaking educational campaigns in churches and screening for liver cancer.
However, he called for more advocacy to educate the public on the disease, saying it could be treated if identified early.
He explained that liver cancer was most prevalent in people between 35 and 45 years, while pancreatic cases were prevalent among people in the 60 to 70-year group.
CEO
When contacted after the surgery, the Chief Executive Officer of the Korle Bu Teaching Hospital, Dr Daniel Asare, commended Dr Offei and the entire Department of Surgery for the introduction of the new procedure.
He said as the Korle Bu Teaching Hospital was inching towards its centenary, the board and the management would intensify the introduction of some sub-speciality services.
That, he explained, was intended to provide services for which Ghanaians would travel abroad.
“This is a new dawn in Korle Bu and more services will be added in the coming years,” he added.
Source: Graphiconline